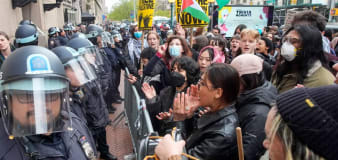news
USA TODAY
Tennessee teacher arrested after bringing guns to preschool, threatening co-worker: Police
CNN
Students at more universities announce solidarity rallies after 108 pro-Palestinian activists are arrested at Columbia
CBS News
Unusual playing cards in Mississippi jails aim to solve cold cases
The Telegraph
French schoolgirl, 14, dies from heart attack during lock-in to protect children from knifeman
Associated Press
FAA investigating after it says a flight told to cross a runway where another was starting takeoff
Advertisement
Stay informed and up-to-date with your local news, breaking news events, global events, savings events, solar eclipse news, and in-depth coverage on a wide range of topics. From politics and technology to entertainment and science, we bring you the latest news from around the world.